Competencies
- AN77.3: Describe spermatogenesis and oogenesis along with diagrams.
INTRODUCTION
- Gametogenesis is the process by which specialized germ cells produce mature gametes through mitotic proliferation, meiotic division, and cellular differentiation. In males, the mature gamete is the spermatozoon, and in females, it is the ovum.
- In males, primordial germ cells migrate to the developing testes during early embryonic life. After reaching the gonads, they remain inactive from approximately the sixth week of intrauterine life until puberty. At puberty, these cells differentiate into spermatogonia. Spermatogonia undergo mitosis to maintain their population and meiosis to form haploid spermatids, which subsequently differentiate into spermatozoa. This process, known as spermatogenesis, continues throughout adult life.
- In females, primordial germ cells differentiate into oogonia within the developing ovaries. By the fifth month of intrauterine life, most oogonia enter the first meiotic division and become primary oocytes. These primary oocytes are arrested in prophase of meiosis I and remain in this suspended state from fetal life until puberty.
- After puberty, during each menstrual cycle, a group of primary oocytes resumes development within ovarian follicles. Usually, only one primary oocyte completes the first meiotic division to form a secondary oocyte and a first polar body. The secondary oocyte begins the second meiotic division but is arrested in metaphase II at the time of ovulation. Completion of the second meiotic division occurs only if fertilization takes place. These cyclical changes continue until menopause, which typically occurs between 45 and 50 years of age.
- Meiosis during gametogenesis reduces the chromosome number from diploid to haploid, ensuring restoration of the normal diploid number at fertilization.
SPERMATOGENESIS
- Spermatogenesis is the process by which male gametes, known as spermatozoa, are produced from spermatogonia.
- It occurs within the seminiferous tubules of the testes.
- The process begins at puberty under the influence of increasing levels of testosterone and continues throughout adult life, including advanced age, although efficiency may decline with age.
- The entire process, from spermatogonium to mature spermatozoon, takes approximately 64 to 74 days. In healthy adult males, about 300 million spermatozoa are produced each day.
Process
- Spermatogenesis takes place in the seminiferous tubules of the testes and can be described in three sequential phases: spermatogonial proliferation, meiotic division, and spermiogenesis.
1. Spermatogonial Proliferation (Spermatocytogenesis)
- This phase involves the transformation of spermatogonia into primary spermatocytes.
- Before puberty, the primitive sex cords develop a lumen and form seminiferous tubules. Primordial germ cells differentiate into spermatogonial stem cells, which remain inactive until puberty.
- At puberty, under the influence of testosterone, spermatogonial stem cells begin active division.
- Type A dark spermatogonia, located adjacent to the basement membrane of the seminiferous tubules, function as stem cells. These cells undergo mitosis to produce type A pale spermatogonia.
- Further mitotic divisions of type A pale spermatogonia give rise to type B spermatogonia (46,XY).
- Type B spermatogonia then divide mitotically to form primary spermatocytes (46,XY), which are the largest germ cells in the seminiferous epithelium. Developing germ cells are supported and nourished by Sertoli cells.
2. Meiotic division
- This phase converts diploid primary spermatocytes into haploid spermatids. Each primary spermatocyte (46,XY) undergoes the first meiotic division to form two secondary spermatocytes (23,X and 23,Y).
- The chromosome number is reduced to half during this division. Each secondary spermatocyte then undergoes the second meiotic division to produce a total of four haploid spermatids (23,X or 23,Y).
- Spermatids are haploid cells and represent the immediate precursors of spermatozoa.
3. Spermiogenesis
- Spermiogenesis is the process by which spermatids differentiate into mature spermatozoa.
- During this phase, the cell undergoes structural reorganization, including condensation of the nucleus, formation of the acrosome, development of the flagellum, and arrangement of mitochondria in the middle piece. This transformation takes approximately 24 days.
- Through these coordinated steps, spermatogenesis produces haploid spermatozoa capable of restoring the diploid chromosome number at fertilization.
Process of Spermiogenesis
- Changes occurring during the process of spermiogenesis are as follows:
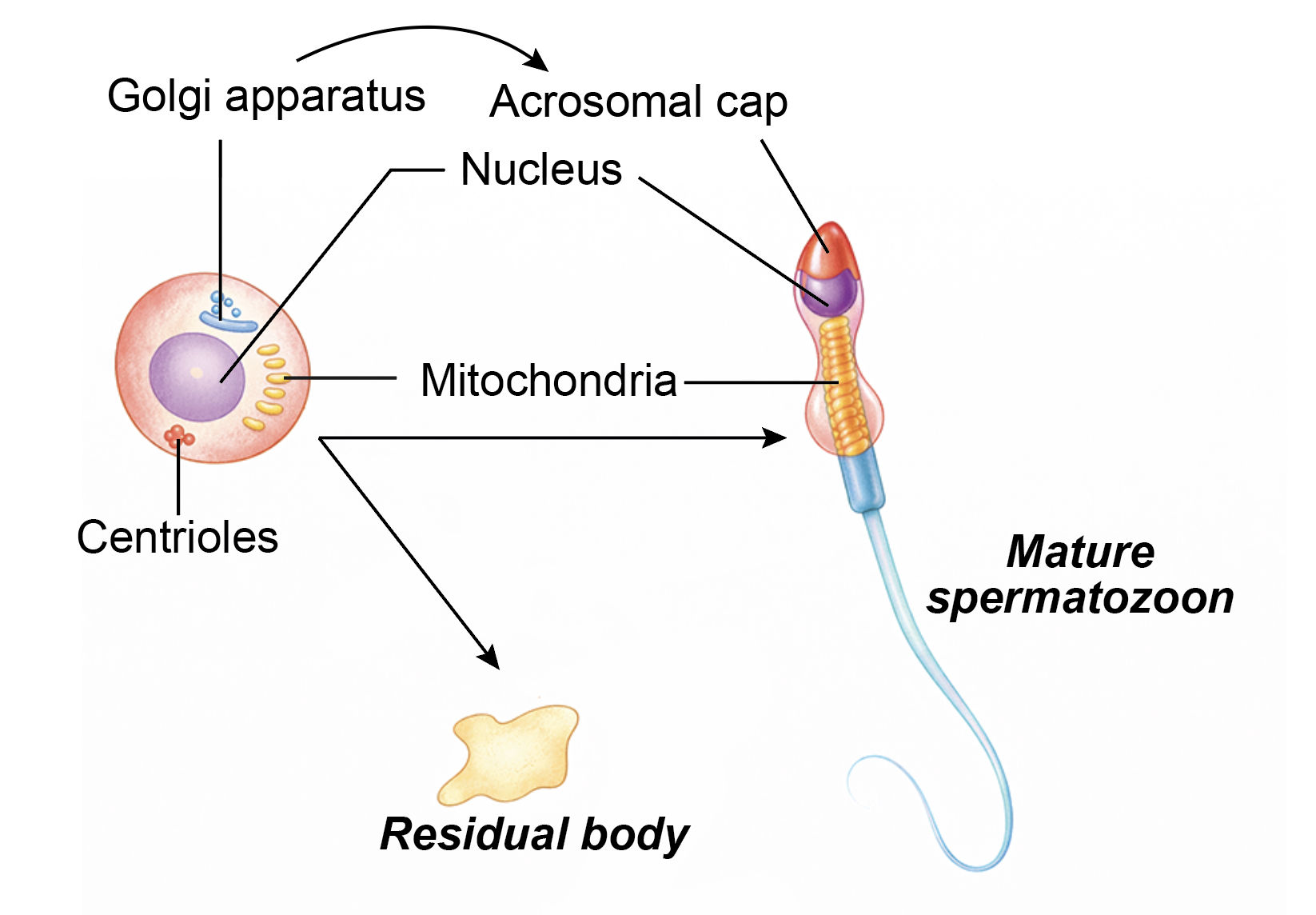
- Nucleus: During spermiogenesis, the nucleus becomes elongated and highly condensed. It shifts toward one pole of the cell, forming the head of the spermatozoon. Chromatin condensation increases genetic stability.
- Golgi apparatus: The Golgi complex produces acrosomal vesicles that fuse to form the acrosome. The acrosome spreads over the anterior two-thirds of the nucleus and contains enzymes required for penetration of the zona pellucida during fertilization.
- Centrioles: The pair of centrioles migrate posterior to the nucleus. The proximal centriole remains near the nucleus in the neck region and contributes to the connecting piece. The distal centriole gives rise to the axoneme, which forms the core of the flagellum and is essential for sperm motility.
- Mitochondria: Mitochondria arrange themselves helically around the proximal part of the flagellum, forming the middle piece. They provide adenosine triphosphate required for tail movement.
- Cytoplasm: Most of the excess cytoplasm is discarded as a residual body. These residual bodies are phagocytosed by Sertoli cells.
- Release of spermatozoa: After structural maturation, the spermatozoa are released from Sertoli cells into the lumen of the seminiferous tubules. This process is known as spermiation.
Spermatogenesis of one sperm:
- Total duration of spermatogenesis is about 64 days; some sources mention 70–75 days as follows:
- Mitotic phase lasts approximately 16 days.
- Meiosis I takes about 8 days.
- Meiosis II takes about 16 days.
- Spermiogenesis requires about 24 days.
Differences between spermatid and spermatozoon
| Spermatid | Spermatozoon |
|---|---|
| It is an immature haploid male germ cell formed after meiosis. | It is a fully differentiated and functionally mature male gamete. |
| The nucleus is relatively large and centrally placed, with less condensed chromatin. | The nucleus is highly condensed and forms the head region of the cell. |
| The Golgi apparatus has not yet formed a definitive acrosome. | The Golgi-derived acrosome is well developed and covers the anterior part of the nucleus. |
| Mitochondria are scattered within the cytoplasm. | Mitochondria are arranged helically around the proximal part of the flagellum, forming the middle piece. |
| It does not possess a flagellum or organized axoneme. | It has a well-developed flagellum with an axoneme that enables motility. |
| It contains a considerable amount of cytoplasm. | Most cytoplasm is eliminated, and only a thin layer remains around the head and tail. |
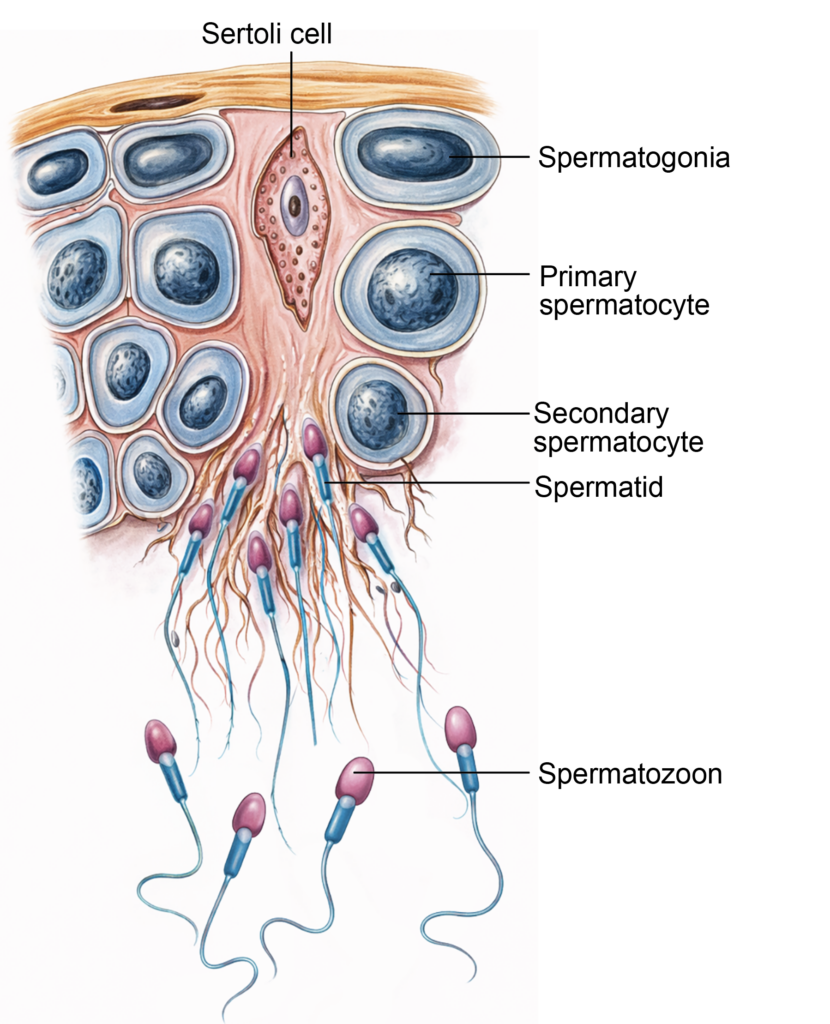
Figure 3.1a: Line diagram: Process of spermatogenesis (Click to see figure)
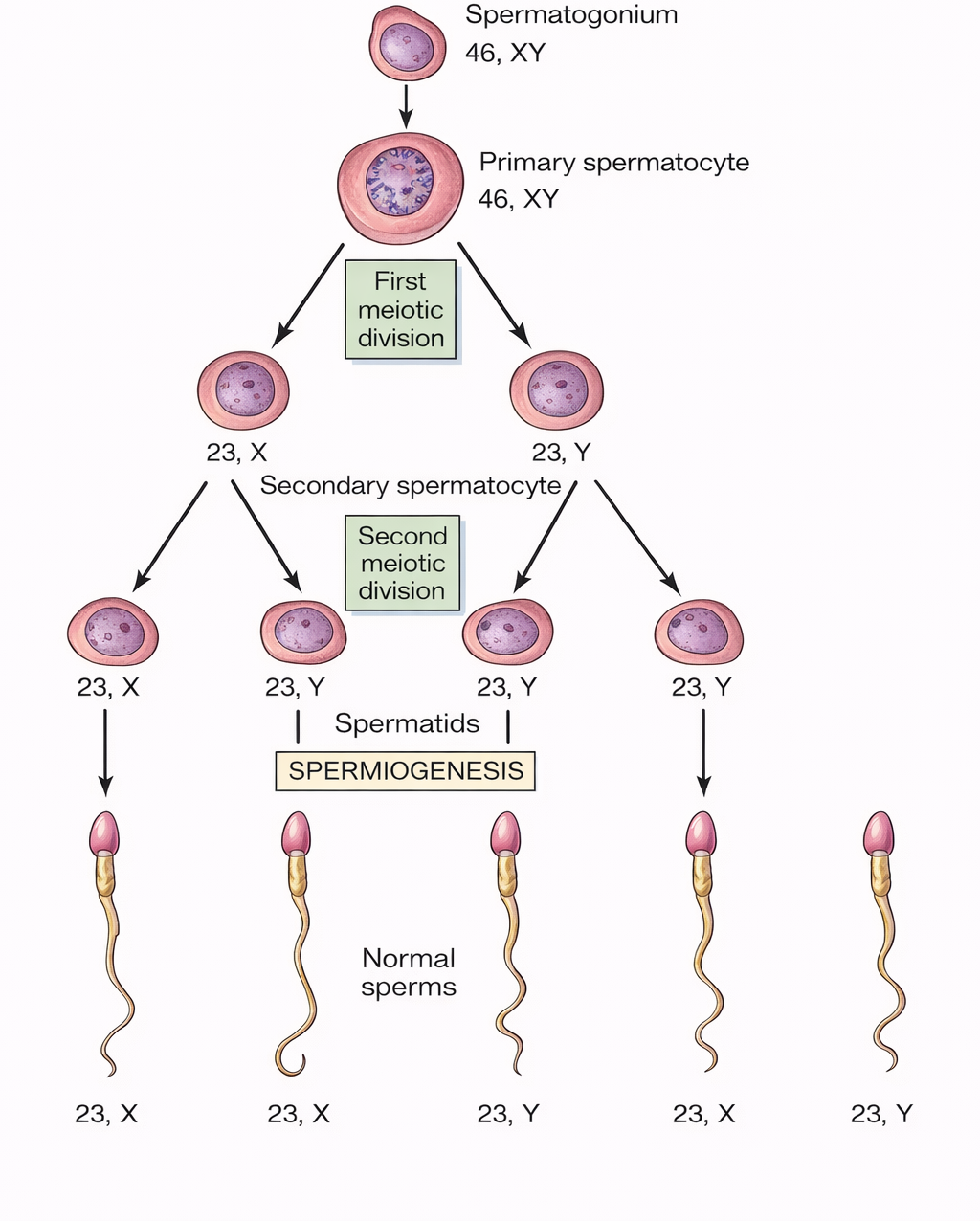
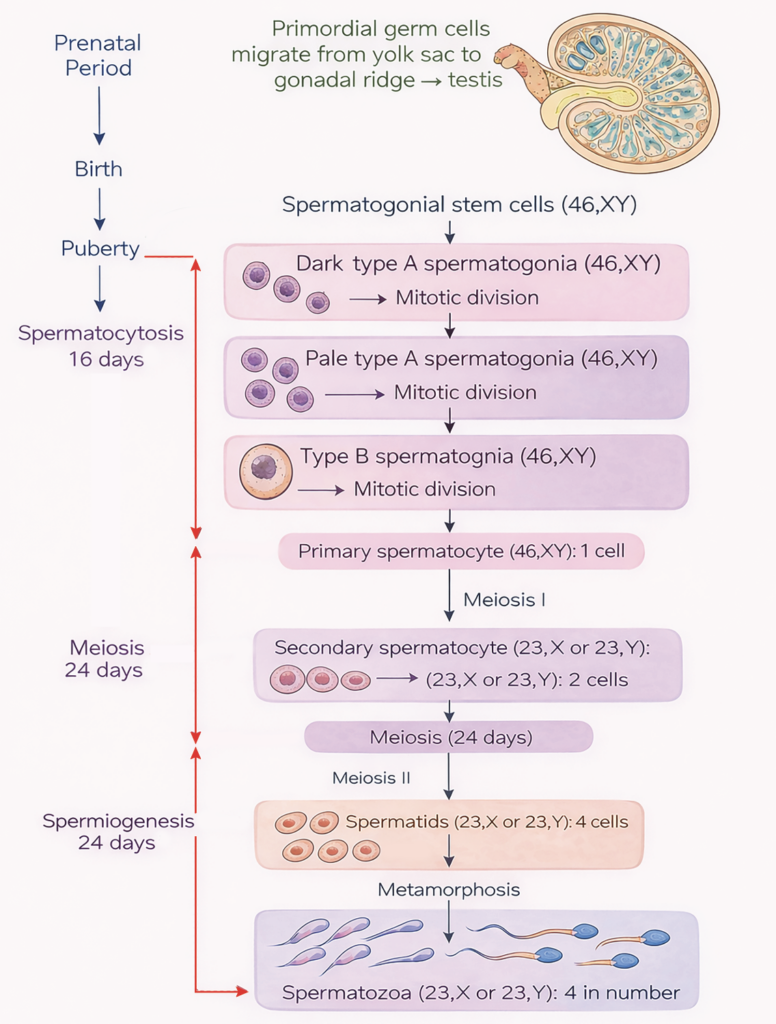
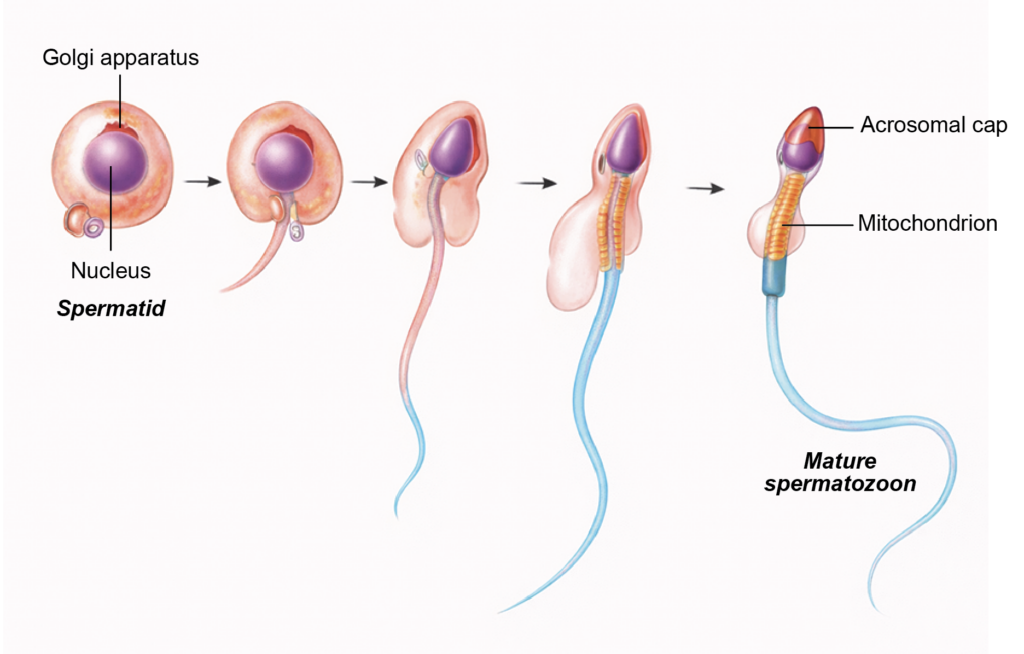
Figure 3.2a: Line diagram: Process of spermiogenesis (Click to see figure)
STRUCTURE OF SPERMATOZOA
- Matured spermatozoa have a head, neck, middle piece and tail.]
- Length: 50–60 μm including head: ~4 m, neck: ~0.3 m, middle piece: ~4 m, tail: ~40 m.
- Count: In a single ejaculation, 200–300 million sperms are emitted in a volume of 2–5 ml semen.
- Life: The usual period of viability after ejaculation is 48 hours, but may survive up to 4 days in the female genital tract.
Parts of Spermatozoon
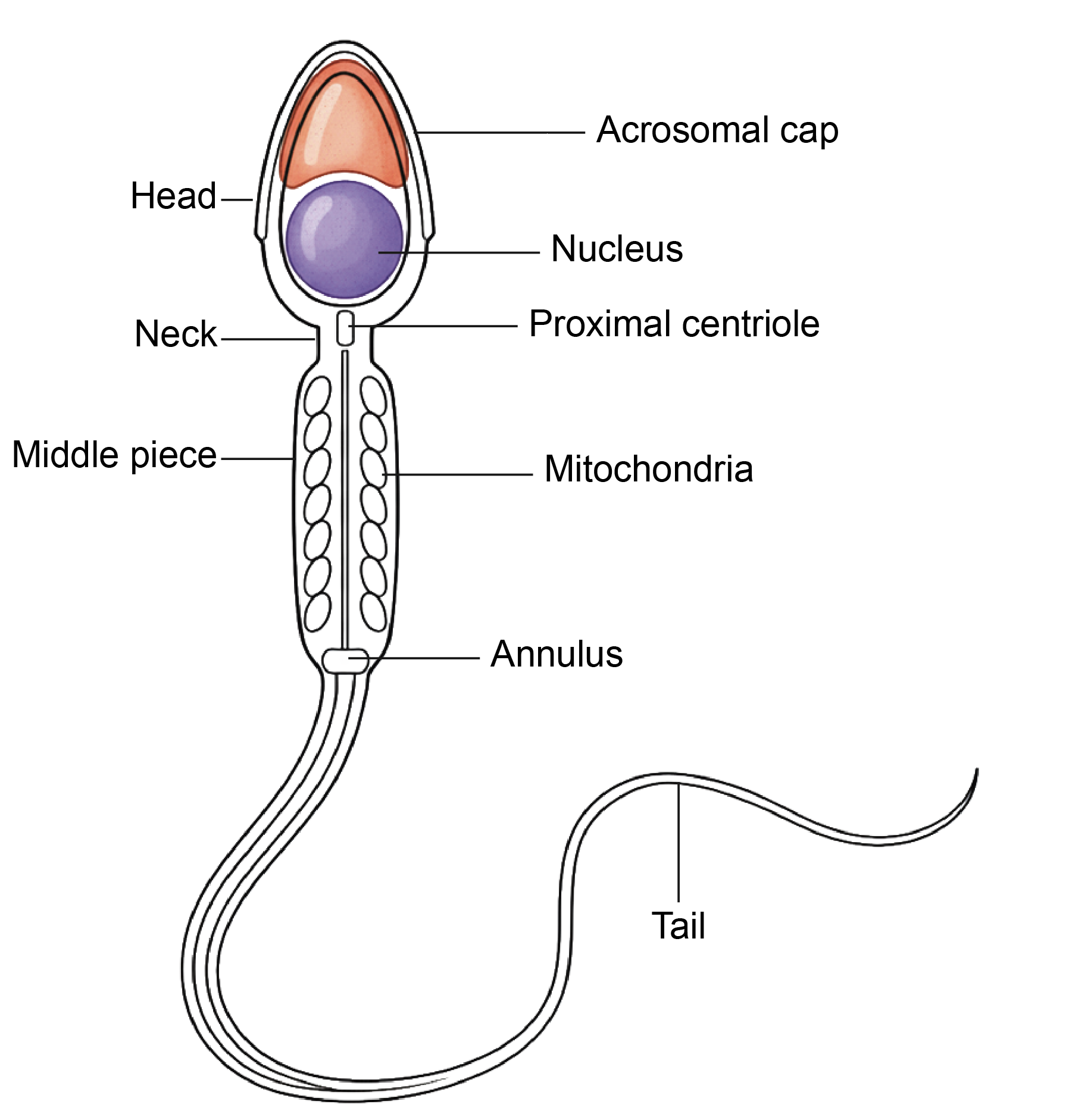
- A spermatozoon is divided into head, neck, middle piece, and tail.
Head
- The head is pyriform in shape. It contains a densely packed haploid nucleus with 23 chromosomes, either X or Y.
- The anterior two-thirds of the nucleus is covered by the acrosome, which is derived from the Golgi apparatus.
- The acrosome contains enzymes such as hyaluronidase and acrosin. These enzymes are released during the acrosome reaction and facilitate penetration of the corona radiata and zona pellucida of the oocyte.
Neck
- The neck connects the head to the middle piece.
- It contains the proximal centriole, which contributes to the connecting piece and plays a role after fertilization in forming the zygotic centrosome. The distal centriole gives rise to the axoneme of the flagellum.
Middle Piece
- The middle piece contains the axoneme, which extends from the neck into the tail.
- The axoneme has a characteristic arrangement of two central microtubules surrounded by nine peripheral doublets.
- Mitochondria are arranged helically around the proximal part of the axoneme, forming the mitochondrial sheath that provides energy for motility.
- An annulus marks the junction between the middle piece and the principal piece.
Tail
- The tail is divided into principal and end pieces.
- In the principal piece, the axoneme is surrounded by a fibrous sheath and plasma membrane.
- In the end piece, only the axoneme and plasma membrane are present.
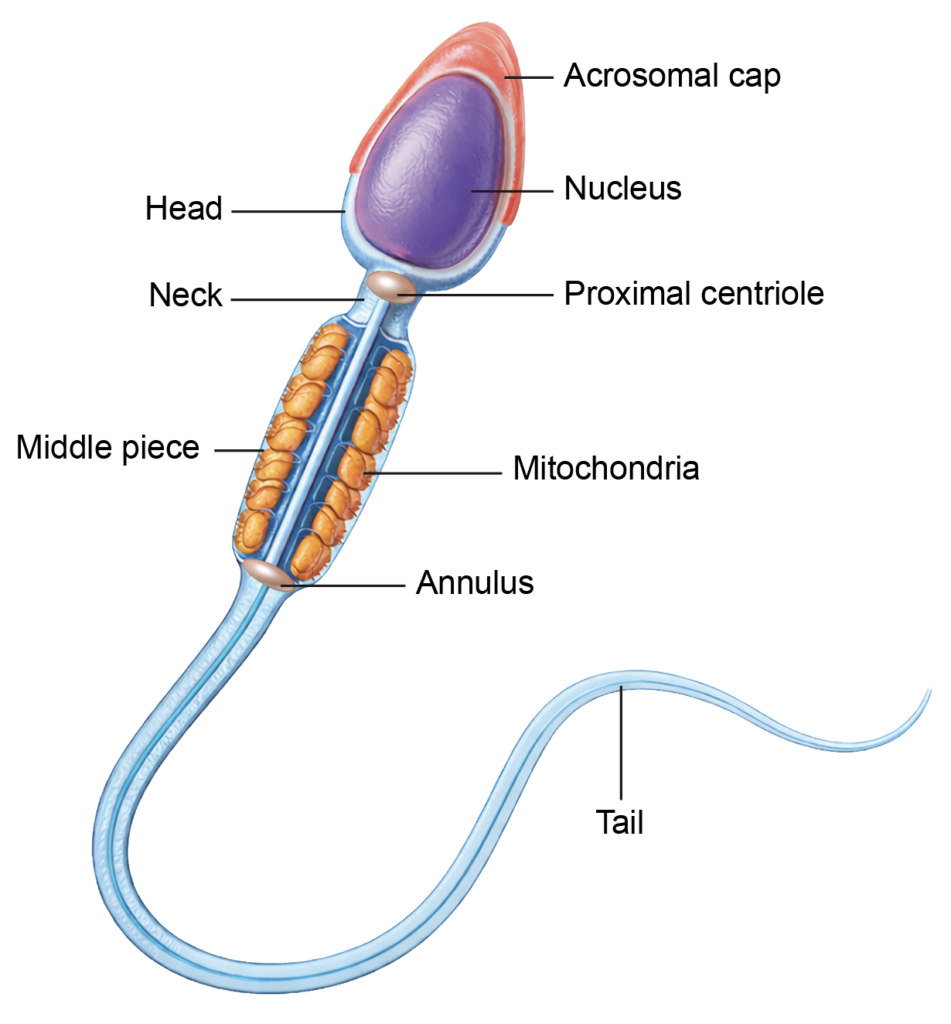
Figure 3.3a: Line diagram: Structure of sperm (Click to see figure)
CLINICAL EMBRYOLOGY
- Abnormal spermatozoa and their counts
- Oligozoospermia: This term refers to a low sperm concentration. According to the World Health Organization criteria, a sperm count below 15 million per milliliter of semen is considered oligozoospermia.
- Azoospermia: This condition is defined as the complete absence of spermatozoa in the ejaculate. It is seen in approximately 1 percent of men and accounts for nearly 20 percent of cases of male infertility.
- Aspermia: Aspermia means absence of semen during ejaculation. It may occur due to retrograde ejaculation, surgical removal of the prostate, or obstruction of the ejaculatory ducts.
- Asthenozoospermia: This condition indicates reduced sperm motility, which can impair the ability of spermatozoa to reach and fertilize the oocyte.
- Hyperspermia and Hypospermia: Hyperspermia refers to an increased volume of semen, whereas hypospermia denotes a decreased semen volume.
- Teratozoospermia: This term describes abnormal sperm morphology. Structural defects may involve the head, middle piece, or tail, such as double heads or abnormal size. In semen analysis of healthy individuals, up to 10 percent of spermatozoa may show morphological variations without necessarily causing infertility.
Capacitation of spermatozoa
- Definition: Capacitation is the functional maturation of spermatozoa that enables them to fertilize an oocyte. This phenomenon was first demonstrated by Chang and Austin in 1951.
- Site: It occurs within the female reproductive tract, mainly in the uterus and uterine tubes.
- Cellular changes during capacitation:
- Removal of seminal plasma proteins attached to the sperm head.
- Modification of the glycoprotein coat over the plasma membrane of the head region.
- Increased membrane fluidity and preparation of the acrosomal membrane for the acrosome reaction.
- Effects of capacitation:
- Enhancement of sperm motility, including hyperactivated movement.
- Destabilization of the acrosomal membrane, which permits enzyme release during the acrosome reaction and facilitates penetration of the zona pellucida of the oocyte.
- Clinical relevance:
- In in vitro fertilization procedures, spermatozoa are processed under laboratory conditions to achieve capacitation.
- In assisted reproductive techniques such as intracytoplasmic sperm injection, a single spermatozoon is introduced directly into the cytoplasm of the oocyte in cases of acrosomal or motility defects.
OOGENESIS
- Definition: Oogenesis is the sequence of cellular events by which primordial germ cells develop into a mature ovum. This process includes mitotic proliferation, meiotic divisions, and cytoplasmic growth.
- Location: Oogenesis occurs in the ovarian cortex, where developing germ cells are enclosed within ovarian follicles.
- Folliculogenesis: It is the gradual growth and differentiation of ovarian follicles. It involves structural and functional changes in both the oocyte and the surrounding follicular cells, ultimately leading to formation of a mature follicle capable of ovulation.
Process of Oogenesis
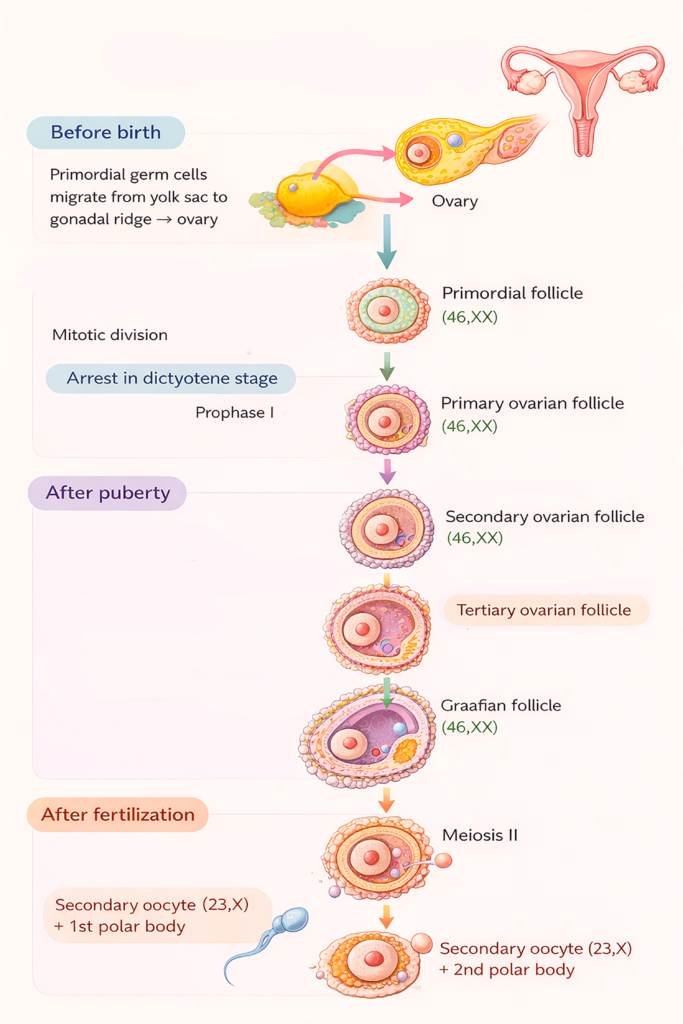
- Oogenesis occurs in three stages: before birth, after puberty, and after fertilization.
Before birth
- During early intrauterine life, primordial germ cells proliferate by mitosis and form oogonia (46,XX).
- By the seventh month of intrauterine life, oogonia enlarge and enter meiosis I to become primary oocytes. These primary oocytes are arrested in the diplotene stage of prophase I under the influence of factors secreted by surrounding follicular cells.
- Each primary oocyte becomes surrounded by a single layer of flattened follicular cells, forming a primordial follicle.
- At birth, about 6–8 lakh primary oocytes are present. This number decreases to around 40,000 by puberty, and fewer than 500 are ovulated during reproductive life.
After puberty
- With the onset of the ovarian cycle, selected primordial follicles resume development.
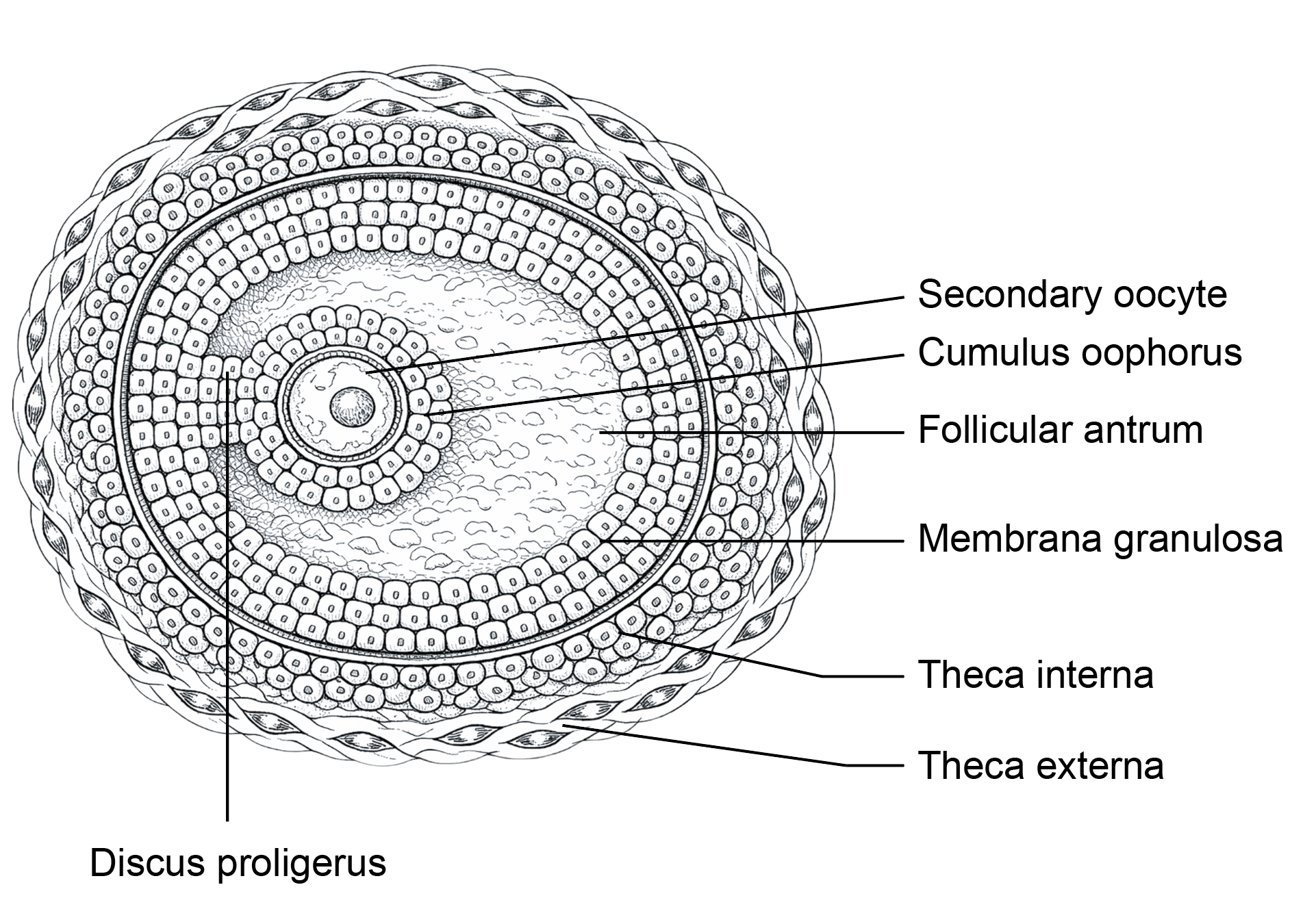
- The follicular cells become cuboidal to form a primary follicle, then proliferate into multiple layers called the granulosa layer, forming a secondary follicle.
- A fluid-filled cavity, the follicular antrum, appears and the follicle becomes an antral follicle.
- Stromal cells differentiate into the theca interna and theca externa; the theca interna secretes estrogen. A glycoprotein layer called the zona pellucida forms around the oocyte.
- Just before ovulation, the primary oocyte completes meiosis I to form a secondary oocyte (23,X) and a first polar body (23,X).
- The secondary oocyte begins meiosis II and is arrested in metaphase II. The mature (Graafian) follicle releases the secondary oocyte at ovulation.
After fertilization
- If fertilization occurs, meiosis II is completed and a second polar body is formed.
- If fertilization does not occur, the secondary oocyte degenerates within about 24 hours. The ruptured follicle transforms into the corpus luteum.
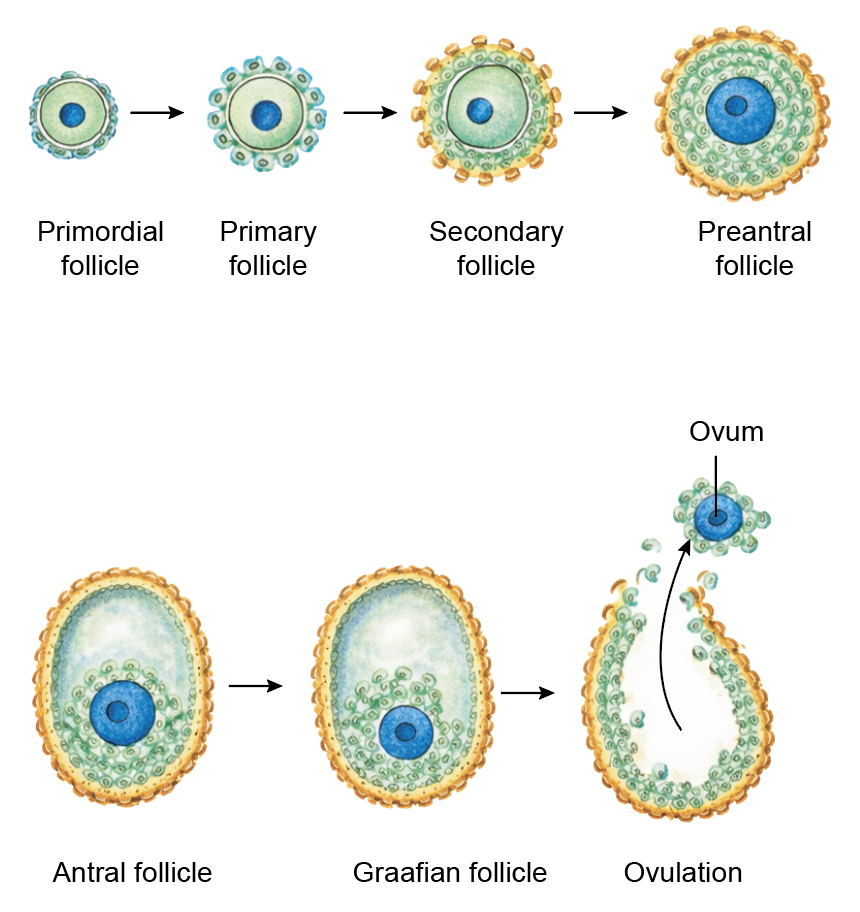
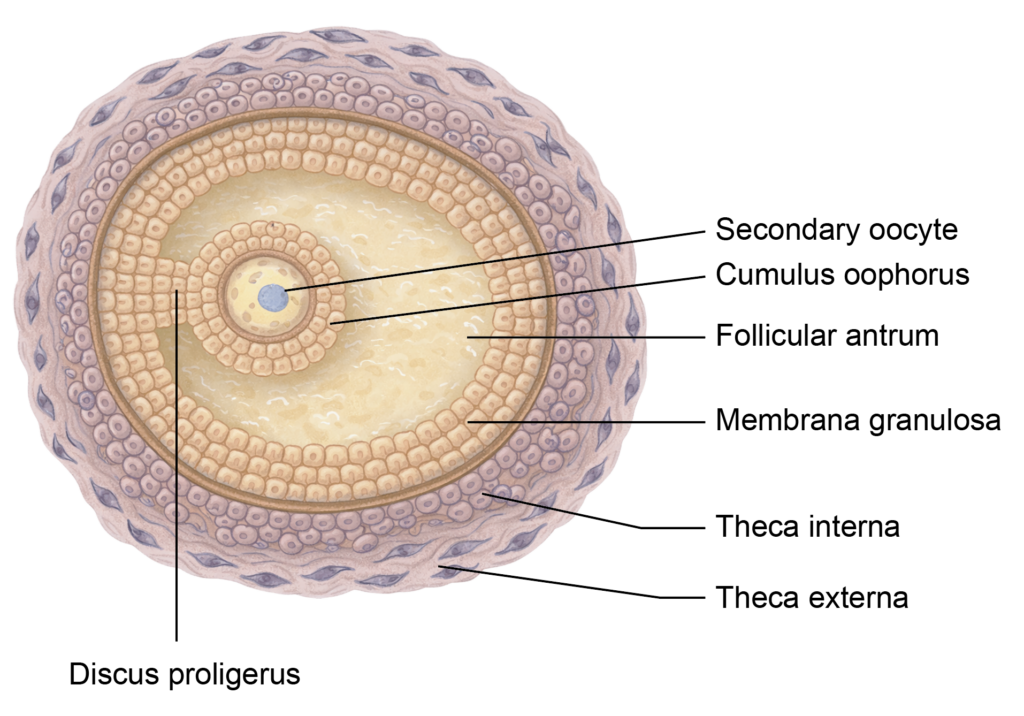
Figure 3.5a: Line diagram: Graafian follicle (Click to see figure)
OVULATION
- Definition: Ovulation is the release of a secondary oocyte from a mature (Graafian) follicle of the ovary.
- Timing: It usually occurs about 14 days before the onset of the next menstrual period. In a typical 28-day menstrual cycle, ovulation takes place around day 14, with a variation of approximately ±1 day.
Factors Responsible for Ovulation
- Luteinizing hormone (LH) surge:
- A rapid rise in luteinizing hormone occurs shortly before ovulation. This surge is the primary trigger for ovulation.
- LH increases the activity of proteolytic enzymes, including collagenase, which weaken the collagen fibers in the wall of the mature follicle. As a result, the follicular wall becomes thin and ruptures.
- Ovulation generally takes place about 36 to 40 hours after the onset of the LH surge, which is accompanied by a rise in follicle-stimulating hormone (FSH).
- Prostaglandins:
- An increase in prostaglandin levels within the follicle contributes to ovulation.
- Prostaglandins promote contraction of smooth muscle fibers in the ovarian wall and enhance local vascular changes, which assist in rupture of the follicle.
- Follicular fluid pressure:
- As the follicle matures, accumulation of follicular fluid increases intrafollicular pressure. This rise in pressure, together with enzymatic weakening of the follicular wall, facilitates release of the secondary oocyte.
Events in Ovulation
- Ovulation is a coordinated sequence of hormonal and structural changes that result in release of the secondary oocyte from the ovary.
- A surge in luteinizing hormone, along with a smaller rise in follicle-stimulating hormone, initiates the ovulatory process.
- The amount of follicular fluid increases, which raises the internal pressure within the mature follicle.
- The ovarian surface overlying the follicle becomes thin and avascular, forming a small bulging area known as the stigma.
- The cumulus oophorus expands as granulosa cells secrete substances rich in hyaluronic acid, loosening their attachment to the follicular wall.
- Enzymatic activity weakens the follicular wall, and increased intrafollicular pressure contributes to rupture.
- The follicle ruptures, and the secondary oocyte, surrounded by the zona pellucida and corona radiata, is expelled into the peritoneal cavity.
- The oocyte is then captured by the fimbriae and enters the uterine tube.
POSTOVULATORY FATE OF OVARIAN FOLLICLE
- After ovulation, the ruptured follicle undergoes a series of structural changes. It transforms sequentially into corpus hemorrhagicus, corpus luteum, and later corpus albicans. Ultimately, it regresses and is replaced by fibrous scar tissue.
Corpus hemorrhagicus
- Immediately following release of the secondary oocyte, the empty follicle collapses.
- Small blood vessels rupture at the site of ovulation, and the follicular cavity fills with blood. This stage is known as the corpus hemorrhagicus.
- The blood clot is gradually resorbed. The granulosa and theca interna cells then proliferate and undergo luteinization, leading to formation of the corpus luteum.
Corpus Luteum
- The corpus luteum is a temporary endocrine structure formed from the ruptured follicle after ovulation.
- It appears yellow due to accumulation of lipid-rich pigment within luteal cells and is responsible for the luteal phase of the menstrual cycle.
- Size: Diameter – 2–5 cm.
Luteinization
- After ovulation, granulosa and theca interna cells enlarge and undergo structural and functional changes known as luteinization.
- During this process, the cells develop abundant smooth endoplasmic reticulum and mitochondria for steroid hormone synthesis.
- Theca interna cells differentiate into smaller theca lutein cells, which produce progesterone and small amounts of androgens.
- Granulosa cells become larger granulosa lutein cells, which secrete progesterone, estrogen, and inhibin A.
Function
- The principal hormone secreted by the corpus luteum is progesterone. Progesterone prepares the endometrium for implantation and supports early pregnancy by promoting decidual changes.
Fate of the corpus luteum
- If fertilization occurs: The implanted embryo secretes human chorionic gonadotropin, which maintains the corpus luteum of pregnancy. Progesterone secretion continues until the placenta assumes this function.
- If fertilization does not occur: The corpus luteum begins to regress about 10 days after ovulation and is replaced by fibrous tissue called the corpus albicans.
- Human chorionic gonadotropin prevents luteal regression.
Corpus Albicans
- If fertilization does not occur, by 10th day after ovulation, corpus luteum gets converted to corpus albicans. It is also called atretic corpus luteum or corpus candicans (albicans = white body in Latin).
- Luteolysis: During the formation of corpus albicans, the cells of corpus luteum are removed by macrophages and fibroblast lay down collagen fibers (white-colored). This process is called luteolysis.
- Finally, the corpus luteum shrinks and results in scar formation.
CLINICAL EMBRYOLOGY
- Disorders of ovulation
- Anovulation: Anovulation refers to failure of release of a secondary oocyte during the menstrual cycle. It commonly occurs in menopause and may also result from endocrine disturbances affecting the hypothalamic-pituitary-ovarian axis.
- Oligo-ovulation: This condition is characterized by infrequent or irregular ovulation. It is often associated with irregular menstrual cycles and hormonal imbalance.
- Induced ovulation: In assisted reproductive techniques, ovulation can be stimulated using medications such as clomiphene citrate or controlled doses of human chorionic gonadotropin. These agents promote follicular maturation and trigger release of the oocyte.
- Suppressed ovulation: Combined hormonal contraceptives inhibit folliculogenesis and prevent the luteinizing hormone surge, thereby blocking ovulation.
STRUCTURE OF OVUM
- The ovum released at ovulation is actually a secondary oocyte arrested in metaphase II of meiosis. It completes meiosis only if fertilization occurs.
- Size: The human ovum measures approximately 120–150 micrometers in diameter and is the largest cell in the body.
- Lifespan: After ovulation, the secondary oocyte remains viable for about 12 to 24 hours if fertilization does not occur.
Structure of ovum
- The ovum, which is a secondary oocyte arrested in metaphase II, has several distinct structural components.
Meiotic spindle:
- The nucleus is not seen as a typical nuclear structure. Instead, it is present as a meiotic spindle of the second meiotic division containing 23,X chromosomes.
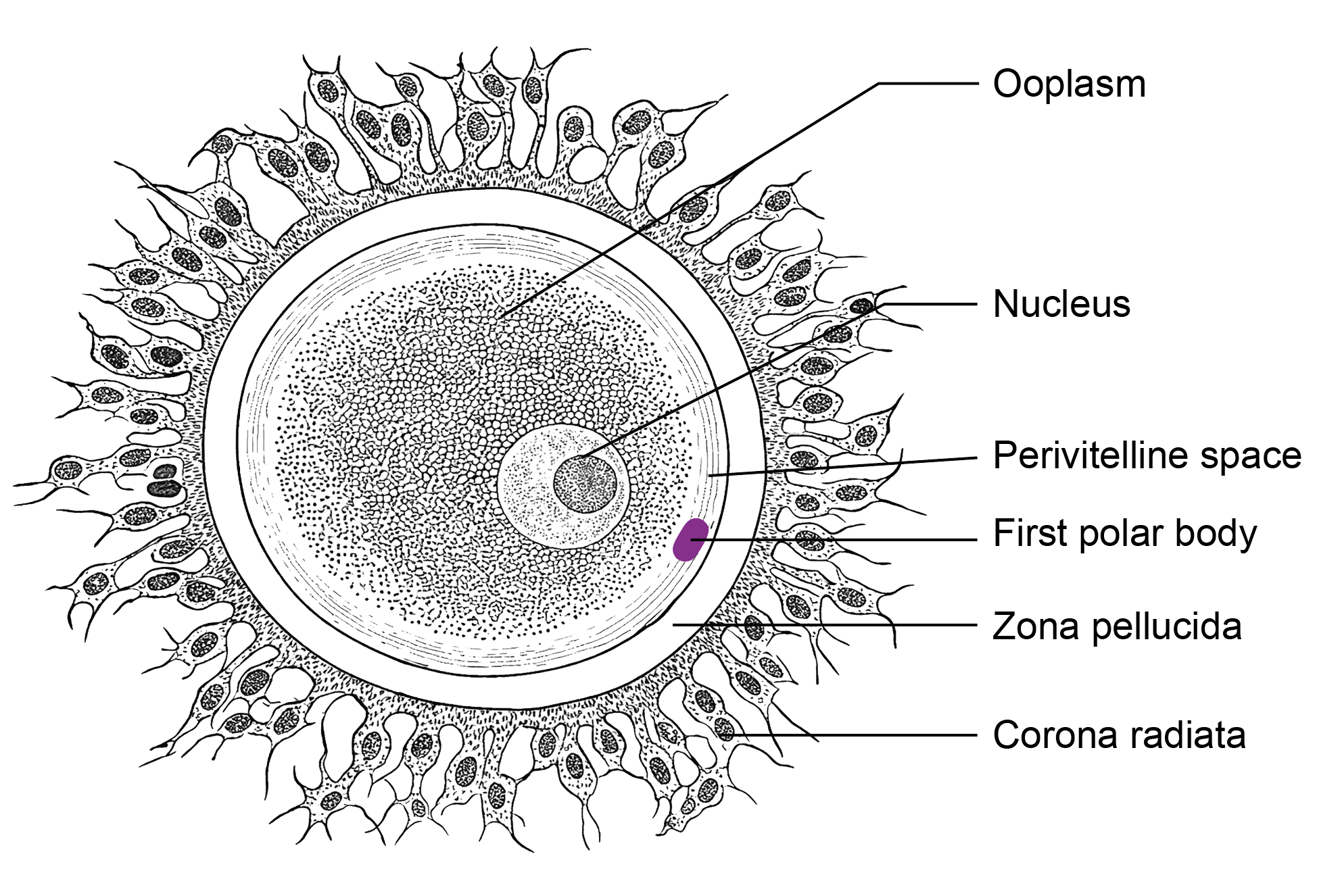
Ooplasm:
- The cytoplasm of the ovum is called ooplasm. It contains organelles, RNA, and nutrient substances. Small yolk-like inclusions, known as deutoplasm, are present and provide support during early embryonic development.
Vitelline membrane:
- This is the plasma membrane of the oocyte. Just outside it lies the perivitelline space, which contains the first polar body.
Zona pellucida:
- This is a thick glycoprotein layer surrounding the vitelline membrane. It plays a role in species-specific sperm binding through glycoproteins such as ZP3, which helps initiate the acrosome reaction.
- The zona pellucida also prevents premature implantation. It degenerates around the fifth or sixth day after fertilization, allowing implantation to occur.
Corona radiata:
- A layer of granulosa cells remains attached to the outer surface of the zona pellucida. These cells form the corona radiata.
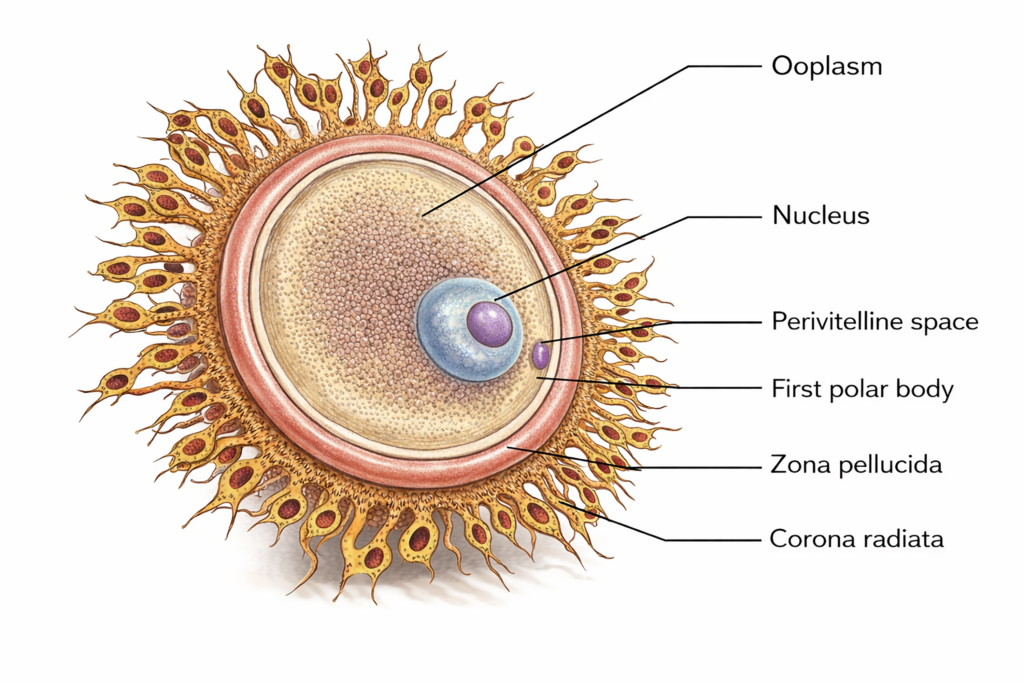
Figure 3.6a: Line diagram: Structure of ovum (Click to see figure)
Differences between sperm and ovum
| Feature | Spermatozoon | Ovum (Secondary oocyte) |
|---|---|---|
| Definition | It is the male gamete responsible for fertilization. | It is the female gamete released at ovulation. |
| Size | It is very small; the head measures about 4–5 µm in length and about 2–3 µm in width. | It is the largest human cell, measuring about 120–150 µm in diameter. |
| Lifespan | It can survive for about 1–3 days in the female reproductive tract. | It remains viable for about 12–24 hours after ovulation. |
| Site of production | It is produced in the seminiferous tubules of the testes. | It develops in the cortex of the ovary. |
| Mobility | It is motile due to the presence of a flagellum. | It is non-motile. |
| Cytoplasm | It contains very little cytoplasm. | It has abundant cytoplasm for early embryonic development. |
| Sex chromosome | It carries either an X or a Y chromosome. | It carries only an X chromosome. |
| Capacitation | It undergoes capacitation in the female reproductive tract. | It does not undergo capacitation. |
| Completion of meiosis | Meiosis is completed before ejaculation. | The second meiotic division is completed only after fertilization. |
Differences between spermatogenesis and oogenesis
| Feature | Spermatogenesis | Oogenesis |
|---|---|---|
| Definition | It It is the process by which male gametes, called spermatozoa, are formed from spermatogonia. | It is the female gamete releIt is the process by which the female gamete, called the ovum, is formed from primordial germ cells. |
| Size | It occurs in the seminiferous tubules of the testes. | It takes place in the cortex of the ovary. |
| Onset | It begins at puberty. | It begins during intrauterine life when primary oocytes are formed. |
| Duration | It continues from puberty throughout adult life, although efficiency may decline with age. | It continues from puberty until menopause. |
| Final output from one primary cell | One primary spermatocyte produces four haploid spermatozoa. | One primary oocyte produces one functional ovum and polar bodies. |
| Second meiotic division | The second meiotic division is completed during spermatogenesis without the need for fertilization. | The second meiotic division is completed only after fertilization. |
| Cytoplasm | Most of the cytoplasm is discarded during maturation. | Most of the cytoplasm is retained in the ovum to support early embryonic development. |
| Number of gametes produced | Millions of spermatozoa are produced daily. | Approximately 400 to 500 ova are ovulated during the reproductive lifespan. |
| Temperature requirement | It requires a temperature slightly lower than core body temperature. | It occurs at normal core body temperature. |
CLINICAL EMBRYOLOGY
- Tests for ovulation
- Ovulation can be identified by clinical observation, hormonal assessment, and imaging techniques.
- Calendar method: In women with regular cycles, ovulation usually occurs about 14 days before the next menstrual period.
- Basal body temperature: Daily early-morning temperature is recorded before any activity. A slight fall of about 0.3–0.5°C may occur just before ovulation, followed by a small rise during the luteal phase due to the thermogenic effect of progesterone.
- Endometrial biopsy: Histological examination of the endometrium can indicate ovulation, but this method is not routinely used now.
- Cervical mucus examination (spinnbarkeit or Billings method): Around ovulation, cervical mucus becomes clear, thin, and stretchable. It can be elongated into a thread of several centimeters and may show a fern-like pattern on drying. This elasticity decreases before and after ovulation.
- Hormonal assessment: A mid-cycle surge in luteinizing hormone, with rising estrogen levels, indicates impending ovulation. Urinary ovulation kits detect the LH surge.
- Ultrasonography: Serial ultrasound monitoring helps track follicular growth and confirm follicular rupture.
- Mittelschmerz: Some women experience mild lower abdominal pain at mid-cycle due to peritoneal irritation from follicular rupture.
- Vaginal discharge or spotting: A temporary increase in discharge or slight spotting may occur at ovulation.
- Note: In modern clinical practice, ultrasonography and LH detection are preferred for accurate ovulation assessment.
- Ovulation can be identified by clinical observation, hormonal assessment, and imaging techniques.
Important Questions
- Write a short note on spermatogenesis.
- Write a short note on spermiogenesis.
- Write a short note on capacitation.
- Write a short note on the structure of spermatozoa or sperm.
- Draw a well-labelled diagram of sperm.
- List the differences between spermatid and spermatozoon.
- Write a short note on oogenesis.
- Write a short note on ovulation.
- List the differences between spermatogenesis and oogenesis.
- Write a short note on structure of ovum.
- List the differences between sperm and ovum.

