Competencies
- AN43.4: Describe the developmental basis of congenital anomalies of face, palate, tongue, branchial apparatus, pituitary gland, thyroid gland, eye. Development of eye is included in this chapter.
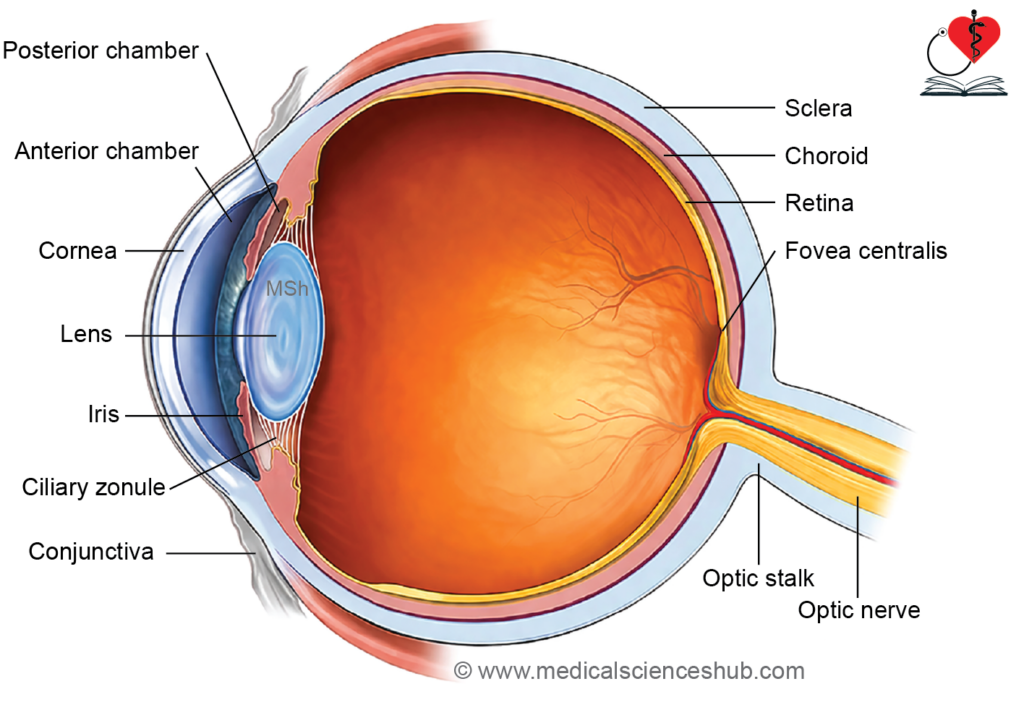
INTRODUCTION
- Development of the eyeball begins early in the 4th week of intrauterine life with the formation of the optic vesicle, an outgrowth from the diencephalon.
- Different parts of the eye arise from distinct embryonic sources:
- The retina, iris, and optic nerve originate from the neuroectoderm of the optic vesicle.
- The lens and corneal epithelium develop from the surface ectoderm via the lens placode.
- The fibrous and vascular coats of the eyeball arise from surrounding mesenchyme.
- The sclera and choroid are largely formed by neural crest cells.
OPTIC VESICLE AND LENS VESICLE DEVELOPMENT
- Optic sulcus formation: Around day 22, a depression appears in the diencephalic wall, forming the optic sulcus, the earliest sign of eye development.
- Optic vesicle formation: The sulcus evaginates laterally into surrounding mesenchyme, forming the optic vesicle.
- Optic stalk formation: The optic vesicle remains connected to the forebrain by the optic stalk.
- Lens placode formation: Contact between the optic vesicle and surface ectoderm induces thickening of ectoderm to form the lens placode.
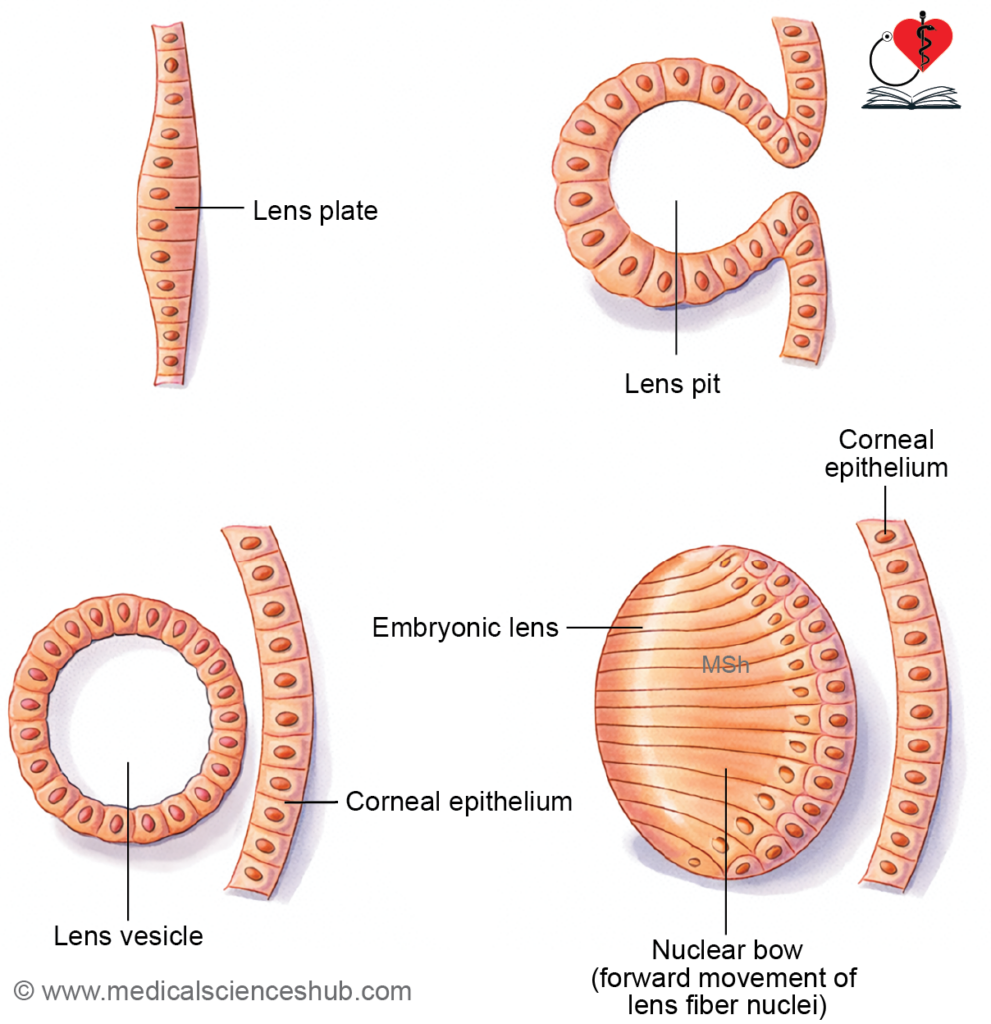
- Lens vesicle formation: The placode invaginates into a lens pit, which separates to form the lens vesicle by approximately day 33.
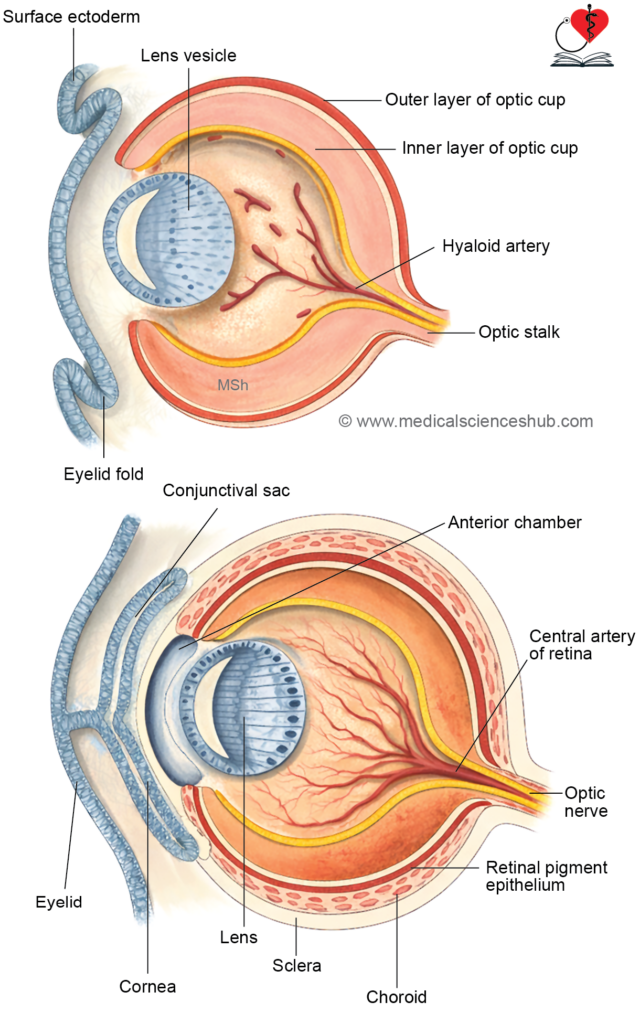
- Optic cup formation: Invagination of the optic vesicle produces a double-layered optic cup. Its margins grow around the lens, leaving an inferior gap called the choroidal (fetal) fissure.
- Hyaloid vessels development: Mesenchyme entering through the fissure forms hyaloid vessels, which supply the developing lens and retina. The distal portions regress, while proximal parts persist as the central artery and vein of the retina.
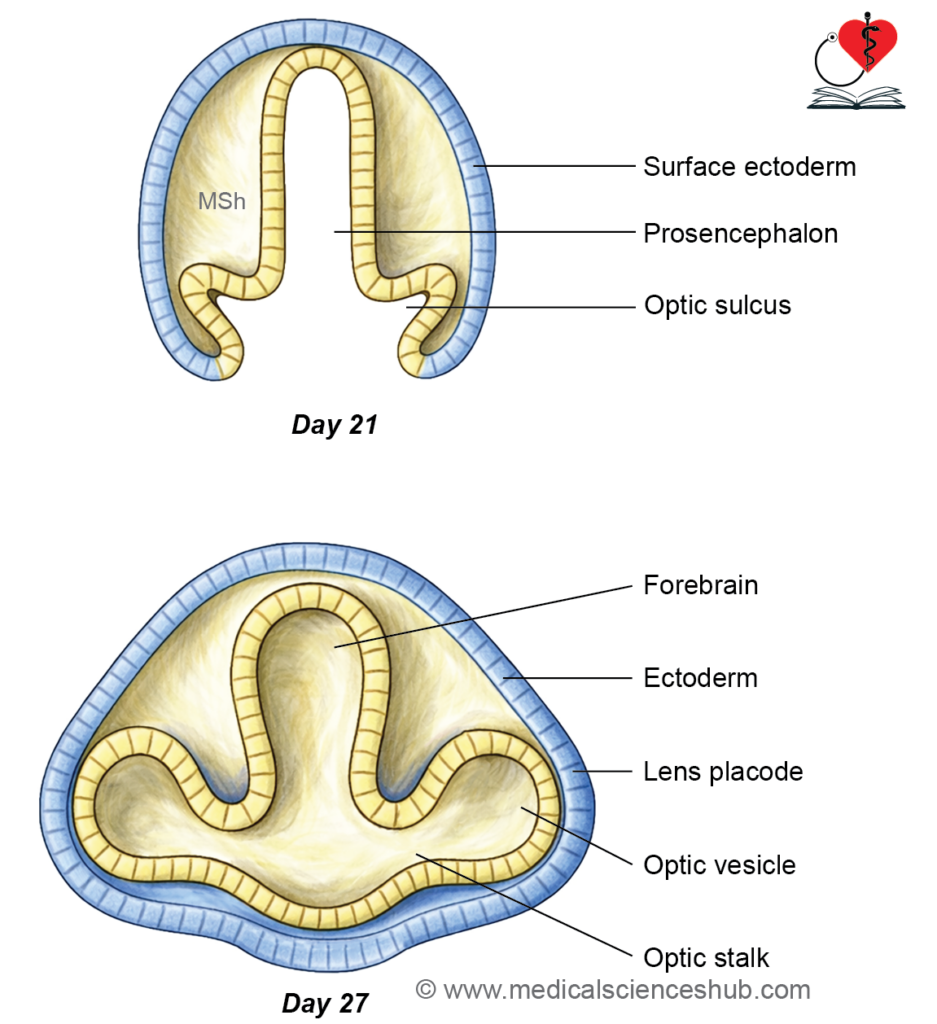
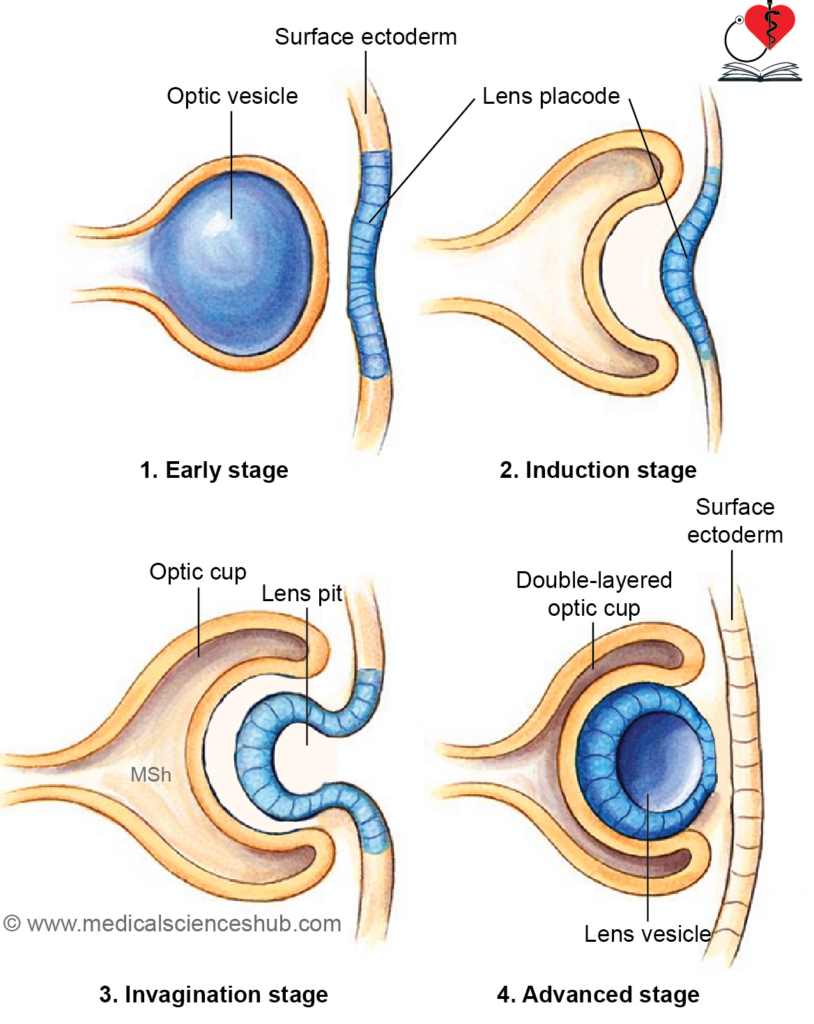
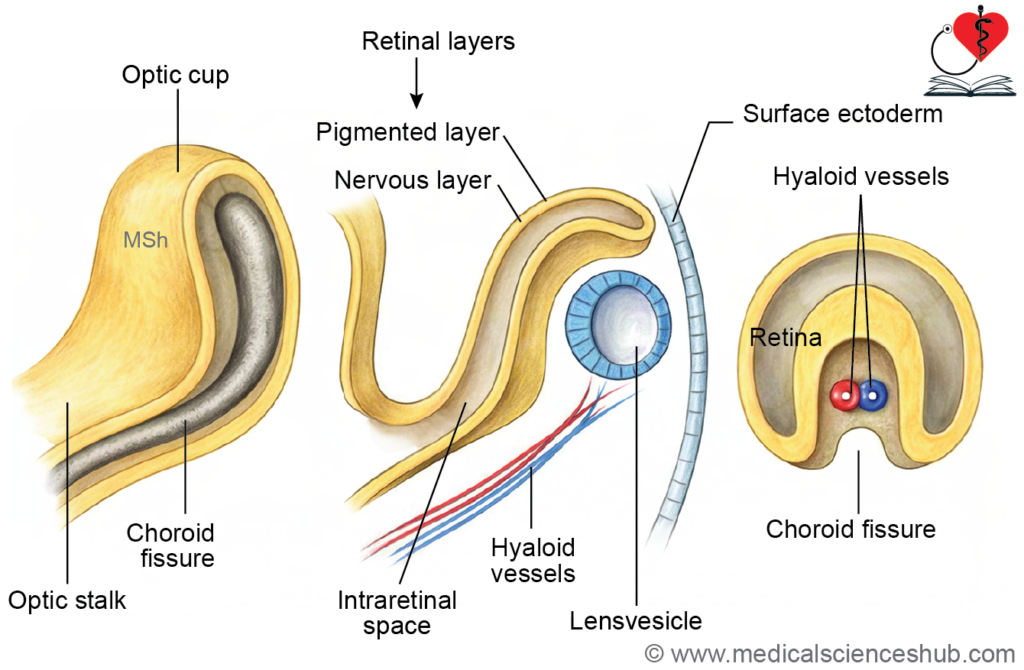
Table 23.1: Development of the Eye (Embryological Origins)
| Structure | Embryological Origin |
|---|---|
| Cornea | Epithelium from surface ectoderm; stroma and endothelium from neural crest cells |
| Lens | Derived from surface ectoderm via the lens vesicle |
| Retina | Develops from the optic cup (neuroectoderm) |
| Optic nerve | Formed from the optic stalk (neuroectoderm) |
| Sclera & choroid | Arise from mesenchyme (neural crest + mesoderm) surrounding the optic cup |
| Ciliary body | Epithelium from neuroectoderm; muscle and stroma from mesenchyme |
| Iris | Stroma from mesenchyme; epithelium from optic cup (neuroectoderm) |
| Iris muscles | Derived from neuroectoderm (unique among muscles) |
| Extraocular muscles | Develop from preotic (preoccipital) myotomes |
| Eyelids & conjunctiva | Formed from surface ectoderm with mesenchymal contribution |
| Lacrimal gland | Originates from surface ectoderm |
| Lacrimal sac & nasolacrimal duct | Develop from ectoderm in the nasolacrimal (naso-optic) groove |
DEVELOPMENT OF VARIOUS PARTS OF EYEBALL
Cornea
- The cornea is a transparent, multilayered structure composed of an outer stratified squamous epithelium, a supporting stroma, Descemet’s membrane, and an inner endothelium.
- These layers arise from two principal embryonic sources:
- The surface ectoderm gives rise to the outer epithelial layer and its underlying basement membrane (Bowman’s layer).
- Neural crest cells migrate to form the corneal stroma (lamina propria), Descemet’s membrane, and the inner corneal endothelium.
- This coordinated development ensures corneal transparency and structural integrity, which are essential for proper light transmission.
Lens
- The lens is a transparent, biconvex structure situated between the aqueous humor and vitreous body of the eye.
- It consists of three main components:
- Lens capsule
- Lens epithelium
- Lens fibers
Stages of Development
- By approximately day 33 of intrauterine life, the lens vesicle separates from the surface ectoderm. Initially, it is lined by a single layer of cuboidal epithelial cells.
- Cells of the posterior wall elongate into columnar cells, fill the cavity, lose their nuclei, and form primary lens fibers, which contribute to lens transparency.
- Cells at the equatorial region continue to proliferate and differentiate into secondary lens fibers, leading to progressive growth and increased density of the lens.
- The anterior wall cells persist as the lens epithelium, maintaining metabolic activity.
- With regression of the hyaloid artery, the lens becomes avascular. By the 7th week, it develops into a solid, fully formed structure.
Retina
- The retina is a multilayered neural structure. From outer to inner side, it includes:
- Pigmented layer
- Photoreceptor layer (rods and cones)
- Bipolar cell layer
- Ganglion cell layer
- All retinal layers are derived from the optic cup, which originates from the neuroectoderm.
Stages of Development
- The optic vesicle arises from the diencephalon and remains connected to it by the optic stalk as it grows laterally.
- Contact with the developing lens induces invagination of the optic vesicle, forming a double-layered optic cup with anterior and posterior regions.
- The anterior part gives rise to the epithelial lining of the ciliary body and iris.
- The posterior part differentiates into retinal layers:
- The outer layer forms the retinal pigment epithelium (RPE).
- The inner layer develops into neural components:
- The matrix layer forms photoreceptors (rods and cones).
- The mantle layer gives rise to bipolar, ganglion, and other retinal neurons.
- The marginal layer contains axons of ganglion cells that converge to form the optic nerve.
- The initial cavity between the two layers, called the intraretinal space, is gradually obliterated as neuronal differentiation progresses.
Optic Nerve
- The optic stalk initially contains the hyaloid artery and vein along with axons from the ganglion cell layer of the developing retina.
- A groove on its inferior surface, the choroidal fissure, allows passage of these vessels and normally closes by the 7th week of development.
- As development progresses, the optic stalk is transformed into the optic nerve, while the hyaloid vessels persist proximally as the central artery and vein of the retina.

Congenital Retinal Detachment
- This condition involves separation of the retinal pigment epithelium (RPE) from the overlying neural retina.
- It is commonly associated with autosomal recessive inheritance and leads to severe visual impairment or congenital blindness.
Sclera and Choroid
- The sclera is a dense, opaque fibrous outer layer that provides structural support and protection to the eyeball. The choroid is a highly vascular middle layer situated between the sclera and the retina.
- During the 6th to 7th weeks of development, surrounding mesenchyme condenses around the optic cup and differentiates into two distinct layers:
- An outer fibrous layer forming the sclera
- An inner vascular layer forming the choroid
- The choroid is continuous anteriorly with the ciliary body and posteriorly blends with the pia and arachnoid mater.
- The sclera continues anteriorly with the corneal stroma (substantia propria) and posteriorly merges with the dura mater surrounding the optic nerve.
Ciliary Body
- The ciliary body is a ring-shaped structure that separates the aqueous humor from the vitreous body and plays a key role in accommodation. It contains the ciliary muscle, which regulates the shape of the lens.
- Its inner surface forms folds called ciliary processes, which secrete the aqueous humor.
- The ciliary muscle and connective tissue develop from surrounding mesenchyme (largely neural crest–derived).
- The epithelial lining has a dual origin from the optic cup:
- The outer layer forms the pigmented epithelium, continuous with the retinal pigment epithelium.
- The inner layer forms the non-pigmented epithelium, continuous with the neural retina.
Iris
- The iris is a thin, circular diaphragm that regulates the size of the pupil and thereby controls light entry into the eye. It consists of an anterior limiting layer, stroma, sphincter and dilator pupillae muscles, and a posterior pigmented epithelium.
- It develops from the anterior extension of the optic cup. The double-layered epithelium of the iris arises from the optic cup, while neuroectodermal cells give rise to the sphincter and dilator muscles.
- The stromal connective tissue is derived from neural crest cells.
- Eye color is determined by the amount and distribution of melanin within the iris, which is genetically regulated.
Anterior and Posterior Chambers of Eye
- The anterior and posterior chambers are fluid-filled spaces of the eye, functionally comparable to the subarachnoid space in maintaining fluid circulation.
- During development, mesenchyme between the cornea and lens cleaves to form a continuous space, which is later divided by the developing iris and pupillary membrane into anterior and posterior chambers.
- With regression of the pupillary membrane, both chambers communicate through the pupil.
- The epithelium of the ciliary processes secretes aqueous humor, which fills these chambers and maintains intraocular pressure.
- At the sclerocorneal junction, mesenchymal tissue forms the trabecular meshwork, which canalizes to form the canal of Schlemm for drainage of aqueous humor.
Vitreous
- The vitreous body is a transparent, gelatinous substance that fills the vitreous chamber and constitutes nearly half of the eyeball’s volume. It maintains ocular shape and supports the retina.
- Its development occurs in stages:
- The primary vitreous forms initially from mesenchymal cells (largely neural crest–derived) and contains the hyaloid vessels.
- It is subsequently replaced by the secondary vitreous, which is secreted mainly by the inner layer of the optic cup and contributions from the developing lens.
- The vitreous is temporarily supplied by the hyaloid artery, which later regresses, leaving a clear, avascular structure.
Accessory Structures of Eyeball
Extraocular Muscles
- Each eye is moved by six extraocular muscles: superior, inferior, medial, and lateral recti, along with superior and inferior oblique muscles. The levator palpebrae superioris elevates the upper eyelid.
- These muscles develop from preotic (preoccipital) myotomes and are innervated by the oculomotor (III), trochlear (IV), and abducens (VI) nerves.
Eyelids and conjunctival sac
- The eyelids arise from folds of surface ectoderm containing underlying mesenchyme, which forms the tarsal plates and connective tissue.
- Eyelashes and associated glands also originate from surface ectoderm.
- The ectoderm lining the inner eyelid and covering the anterior eyeball forms the conjunctival sac.
- Eyelids remain fused until approximately the 28th week of intrauterine life, after which they separate.
Lacrimal apparatus
- The lacrimal apparatus includes the lacrimal gland, lacrimal sac, and nasolacrimal duct.
- The lacrimal gland develops from multiple ectodermal buds arising in the superolateral conjunctival region.
- The lacrimal sac and nasolacrimal duct form from the nasolacrimal (naso-optic) groove.
- The lacrimal canaliculi develop from canalized ectodermal cords near the medial eyelid margins and later connect with the lacrimal sac.
CLINICAL EMBRYOLOGY
CONGENITAL ANOMALIES OF EYE
1. Congenital Cataract
- Congenital cataract is a lens opacity present at birth and may affect one or both eyes.
- Common causes include intrauterine infections (e.g., rubella, toxoplasmosis), chromosomal abnormalities such as Down syndrome, and metabolic disorders like galactosemia.
- Early surgical removal, especially before 10 weeks in bilateral cases, is essential to prevent visual impairment.
2. Developmental Anomalies
- Anophthalmia: Complete absence of the eye due to failure of optic vesicle formation.
- Microphthalmia: Abnormally small eye caused by defective development of the optic vesicle; often linked to infections or PAX6 gene mutations.
- Cyclopia (Synophthalmia): Formation of a single median eye due to fusion of optic vesicles, associated with impaired SHH (sonic hedgehog) signaling.
- Coloboma of iris: Inferior defect in the iris resulting from incomplete closure of the choroidal fissure, producing a keyhole appearance.
- Persistent pupillary membrane: Remnants of the fetal membrane partially or completely covering the pupil.
- Congenital aniridia: Partial or complete absence of the iris due to abnormal optic cup development.
- Congenital aphakia: Absence of the lens caused by failure of lens vesicle formation.
- Coloboma of eyelid: Partial absence of eyelid tissue due to defective development.
- Optic nerve coloboma: Associated with mutations in the PAX2 gene, often accompanied by renal anomalies.
- Entropion and ectropion: Inward or outward turning of the eyelids, respectively.
- Epicanthus: A skin fold extending from the upper eyelid to the medial canthus, commonly seen in Down syndrome.
- Cryptophthalmos: Absence of eyelids, with skin covering the eyeball.
- Congenital ptosis: Drooping of the upper eyelid due to defective development of the levator palpebrae superioris muscle.

